Ms Julie Kohls
Consultant Orthopaedic Surgeon




Baumann
Gastrocnemius Release
The Gastrocnemius muscle sits at the back of calf and joins another muscle (the soleus) to form the Achilles tendon. People who have gastrocnemius muscle tightness do not have a full range of motion in their ankle when their knee is straight.
Gastrocnemius tightness prevents many structures in the foot and ankle from functioning normally. The abnormal biomechanics caused by gastrocnemius tightness is the root of many foot and ankle conditions especially if the gastrocnemius is part of a “tight chain” at the back of the entire leg.
In patients with very rigid gastrocnemius tightness, I find that the most effect release is to release the gastrocnemius along the deep side of the muscle just before it inserts onto the Achilles tendon.
What can I expect on the day of surgery?
-
The surgery will normally be under a general anaesthetic combined with a local anaesthetic (for later comfort).
-
This is a day surgery case.
-
There will be a bulky bandage on your knee which you will keep dry.
-
You will wear a removable boot (Aircast boot) over your dressing when you are standing and walking.
-
The outer bandage will be removed after 48 hrs but the adhesive dressing underneath must be kept clean.
-
You will be given crutches.
-
You will be started on blood thinners.
What are the risks and complications?
The vast majority of patients do extremely well. A small group of patients need extra physio due to swelling . Complications include infection, DVT, nerve damage, wound healing problems, recurrence,
You must stretch several times a day to encourage the muscle and its covering to heal longer following the surgery.
Clear Advice About DVT
A DVT is a Deep Vein Thrombosis or a blood clot in the leg. A blood clot occurs after PMGR surgery for about 1 in every 100 patients. You can help prevent a blood clot by keeping your knee and ankle and toes moving. Keeping yourself hydrated is also helpful to prevent a DVT. Finally elevating your leg to the level of your heart will minimise the amount of swelling you have which will also help to prevent a DVT.
We will discuss medicines to help prevent a DVT. Most patients have injections of blood thinners for the first two weeks.
If you were the patient who developed a DVT you would likely have some symptoms:
-
The leg (above the dressing/foot) would become hard, heavy, swollen, painful and/or red.
-
If you were to have any of the above symptoms you would have to have a scan to look for a blood clot and then be treated with blood thinners.
If the blood clot were to move to the lungs you would have a pulmonary embolism which is a medical emergency.
-
The symptoms of a pulmonary embolism are breathless & chest pain- Call 911.
When can I drive?
The best guide that you are safe to return to driving is that you are able to walk well without crutches . The usual time scale also depends on whether you had surgery on your right or left foot and whether you drive a manual or an automatic.
-
Right side surgery and all car types: 2 weeks
-
Left side surgery and manual car: 2 weeks
-
Left side surgery & automatic car: 0-1 week
BAUMANN GASTROCNEMIUS RELEASE
How long will I need to off work?
The time you require off from work depends on what type of job you do. If you work on your feet all day, do a manual job, or are required to wear dress shoes you may need 2-3 weeks before you are back at work. If you can work from home or do a sedentary job and can have some support after surgery getting to and from work, you may be able to go back to work after a few days off.
What instructions will I have for the first 2 weeks after surgery?
-
Elevate leg level to heart (above if swollen)
-
Keep kne dry for 2 weeks
-
Reduce Bulky dressing at 48 hours
-
Keep adhesive dressing intact for 2 weeks
-
Move Knee and Ankle
-
Do gastrocnemius stretches
-
Weightbear

Self Exercises
-
Start to stretch the Gastrocnemius Muscle as soon as you can after surgery. Start in bed by wrapping a towel around the foot and pulling the foot upwards while keeping the knee straight. Hold the stretch for as long as you can gradually working up to one minute.
-
Progress to using a theraband for resistance as shown
-
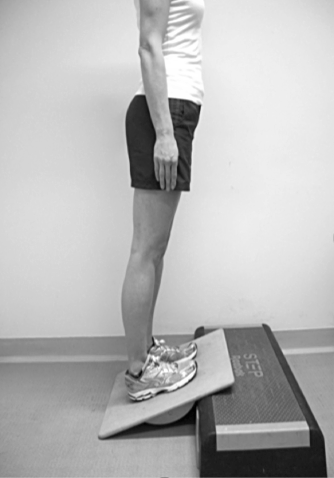
As soon as you can go back to doing standing stretches on the slant board you should. Although the back of the leg will feel bruised following the surgery, no harm can be done by stretching. Put the slant board at its lowest level. Push your body weight forward when you stand on the slant board so that you really feel the stretch in the back of the calf.