
Ms Julie Kohls
Consultant Orthopaedic Surgeon




Achilles Tendon Rupture
What is an Achilles Tendon Rupture?
The Achilles tendon is the strongest tendon in the body. A healthy Achilles tendon can withstand loads up to 10X body weight. When the Achilles tendon ruptures, most patients hear a snap or a pop as well as feeling pain at the back of the ankle. The rupture occurs during sudden forceful acceleration or deceleration during sporting activities.
Following rupture I may advise you that you don’t need surgery because:
-
The ruptured tendon ends come together well when your toes point down
-
You have a partial rupture
What is an Accelerated Rehabilitation?
Rehabilitation of the Achilles tendon has been shown to be be better when patients are able to walk on the affected leg for most of the healing time. Weightbearing (provided the foot is held at the right angle to keep the tendon ends together) encourages healing of the tendon. For patients who do not require surgery, it is still ideal that the tendon ends are allowed to rest in the healing position for a few weeks prior to being put into a boot for weight bearing.
ACCELERATED REHABILITATION
-
I will examine you and confirm you have an acute Achilles rupture and its location
-
You will have an ultrasound to confirm that your tendon will heal
-
You will be in a plaster backslab for two weeks
Why do some patients require surgery prior to starting Accelerated Rehabilitation?
Following rupture I may advise you that you do need surgery because:
-
The ruptured tendon ends do not come together well when your toes point down
-
You are extremely active
-
Your injury was missed for a period and treatment has started late
What can I expect on the day of surgery?
-
The surgery will normally be under a general anaesthetic.
-
This can be a day surgery case.
-
I will numb the ankle with local anaesthetic
-
You will be in a half plaster cast
-
I will give you advice on the number of weeks to take off work
What are the risks and complications?
The vast majority of patients do extremely well. There are risks that occur as a result of an Achilles tendon injury and these risks are: DVT (see below), weakness, and re-rupture of the Achilles tendon.
The risks following surgery on the Achilles tendon are: a small group of patients need extra physio due to swelling or stiffness, infection, slow wound healing, blood clots (DVT) and re-rupture.
When can I drive?
The best guide that you are safe to return to driving is that you are able to walk well without crutches. The usual time scale also depends on whether you had an Achilles tendon rupture on your right or left foot and whether you drive a manual or an automatic
-
Right side and all car types: 8 weeks
-
Left side and manual car: 8 weeks
-
Left side & automatic car: 2 weeks
How long should I take off work?
The time you require off from work depends on what type of job you do. The first two weeks of healing are critical and so you must have this time off work. Many people are able to work from home and so if you can avoid commuting in the first two- four weeks, you will find that your ankle swells less and does better. If your employer can be flexible with your activity at work you may be able to do some lighter duties or reduced hours from 3 weeks onward. If you work on your feet all day, do a manual job, or are required to wear dress shoes you may need 8 weeks before you are back at work.
Clear Advice About DVT
A DVT is a Deep Vein Thrombosis or a blood clot in the leg. A blood clot occurs after surgery where patients are placed into plaster or a splint for about 2 in every 100 patients. You can help prevent a blood clot by keeping your knee moving. Keeping yourself hydrated is also helpful to prevent a DVT. Finally elevating your leg to the level of your heart will minimise the amount of swelling you have which will also help to prevent a DVT. You will be given blood thinners for the first two weeks when you at your least active.
If you were to develop a DVT you would likely have some symptoms and so it is very helpful if know what to look for:
-
The leg (above the dressing/foot) would become hard, heavy, swollen, painful and/or red
-
If you were to have any of the above symptoms you would have to have a scan to look for a blood clot and then be treated with blood thinners
If the blood clot were to move to the lungs you would have a pulmonary embolism which is a medical emergency
-
The symptoms of a pulmonary embolism are breathless & chest pain- Call 999
More Info
-
Summary about the Vacoped Boot
-
Clinical trial demonstrating better results with the Vacoped Boot
Accelerated Rehabilitation of the Achilles Tendon
Instructions 0-2 Weeks
-
Elevate Leg Above Heart
-
Keep dry for two weeks
-
Low-Molecular-Weight Heparin Injection daily (Clexane 40mg)
-
Non weight bearing in plaster back slab
-
Move toes and knee
At 2 Weeks
-
If you have had surgery, I will arrange to have your plaster and sutures removed and to check your wound
-
You will be placed in a Vacoped Boot locked in equinus - toes pointing down
-
You must progress to weight bearing fully in the Vacoped Boot
-
In clinic we will check to make sure that the Vacoped Boot does not rub on the surgical site or your ankle
-
You must wear the Vacoped Boot for all weight bearing activity (standing walking)
-
You will be able to wash the ankle out of the Vacoped Boot but you must keep the ankle pointing down
-
You should schedule your first physiotherapy session for 2 wks
-
If you have had surgery you may remove Vacoped Boot at night but toes must point down and not be forced up by the bed clothes
-
If you have not had surgery it is ideal that you keep the boot even at night until you reach 4 weeks following injury

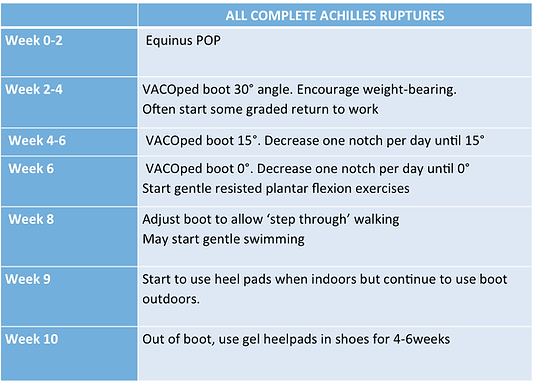

Physiotherapy Instructions 2 Weeks onward
-
These instructions may be best discussed with your physiotherapist
-
Can start active ROM exercises at 2 weeks but only in plantar flexion and non weight bearing
-
Proprioception
-
No forcing/ no stretching/ no active Dorsiflexion (emphasis on keeping Achilles tendon in shortened position)
-
Can commence calf raises in loosened Vacoped Boot (sit in chair wearing loosened boot, go up and down on tip toes to the extent that the boot will allow
-
Active knee, hip exercises
-
Isometric exercises, intrinsic toe exercises, pointing toes, eversion-inversion (in plantar flexion)
-
Work on Soft Tissues:
-
Local modalities
-
Ice/ contrast bathing
-
Soft Tissue Massage
4 Weeks
-
Start gentle cycling- no resistance with high seat
5 Weeks
-
Start weight bearing soleus stretches in boot
6 Weeks
-
Add resistance when cycling
-
Theraband resistance training
7 Weeks
-
Start standing proprioception
-
Progress stretches by removing wedge when stretching and standing bare foot
-
At 9 weeks progress to the 'Surrey Stages' Strengthening Program

Guide to Using Vacoped Boot
Guide to Using Air Cast Boot and Wedges
THE ‘SURREY STAGES’ PHYSIOTHERAPY STRENGTHENING PROGRAM
BRONZE AWARD
DOUBLE HEEL RISES (DHR)
-
You can go up and down on tiptoes in sets of 3, slowly and 15 reps in each
-
You can stand on a skipping rope and adjust your foot position
-
You can hold a DHR for 15 seconds
-
It can be difficult to progress to the next award level because the ankle will take double the weight when you move to lifting the good leg to lower only on the operated leg.
-
You are better to stay at the bronze award level but to add in a back pack with increasing weight as you feel ready for more
-
When you have done this for some time you will be ready to progress to the silver award level
SILVER AWARD
DOUBLE HEEL RISES WITH A LIFT
-
May need to add weight in backpack on DHR to reach silver level
-
You go up on both feet but lift unoperated leg and lower slowly only on operated leg
-
3 sets, working up to 15 reps in each
-
You can stand both feet on a wobble board
-
You can hold a solid DHR for 20 seconds
GOLD AWARD
SINGLE HEEL RISES
-
3 sets, working up to 15 reps in each
-
You can stand on one foot on wobble board
-
You can hold a solid DHR for 40+ seconds
PLATINUM AWARD
-
Progress to hopping in all directions
-
Double Hops
-
Gentle jogging to reintroduce running